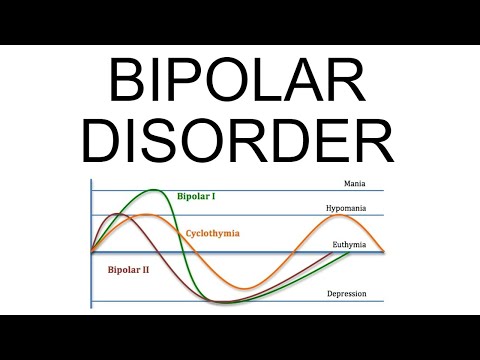
Hey! So, let’s talk about Bipolar 2 Disorder. You know, it’s one of those things that can be a bit hard to wrap your head around. It’s not just having ups and downs like everyone does.
It’s more complex than that. Seriously, imagine being on this emotional rollercoaster, where the lows are really low and the highs don’t quite reach the peak like in other types of bipolar disorder.
If you or someone you know is curious about this, hang tight! We’re diving into what the DSM-5 says about it and breaking it down in a way that makes sense. Trust me, it’ll help clear up some confusion!
Understanding Bipolar Type 2: A Comprehensive Guide to Symptoms and Explanation
Bipolar Type 2 disorder can be kind of tricky to understand. You’ve probably heard about the ups and downs with bipolar, but Type 2 has its own unique flavor. Basically, you’ll see periods of depression and hypomania, which isn’t as intense as full-blown mania found in bipolar 1.
So here’s the deal: in **Bipolar Type 2**, you experience at least one major depressive episode and at least one hypomanic episode. A major depressive episode might feel like you’re trudging through mud every day. You might have lost interest in things you usually enjoy, feel super tired or honestly just numb.
Now, let’s break down those hypomanic episodes! They’re not quite mania but can still feel pretty awesome. You might feel more energized or creative, and your ideas could be flowing like crazy! But this can also lead to risky behaviors or feeling easily annoyed.
In terms of the DSM-5 criteria—which is basically the go-to guide for mental health professionals—here’s what they look for:
- Symptoms of Depression: For a major depressive episode, it usually means having five or more symptoms for at least two weeks.
- Hypomania Symptoms: It’s important to have at least three symptoms present during a hypomanic episode that last for at least four consecutive days.
- Impact on Daily Life: These episodes shouldn’t be explained by another mental health issue or substance use.
Imagine someone named Alex. Alex has been feeling down for weeks—no energy, no motivation to get off the couch. Then suddenly, out of nowhere, Alex gets this burst of energy! It’s like flipping a switch—ideas are racing, sleep feels optional, and everything is exciting again. This is that hypomanic phase kicking in.
But here’s where it gets complicated: these feelings don’t always lead to a happy ending. The highs can quickly turn into lows once that energy fades away again. So there can be this roller coaster effect that leaves you feeling pretty depleted.
You know what’s key? Getting help! Therapy options like Cognitive Behavioral Therapy (CBT) often work wonders because they help tackle those negative thought patterns head-on while providing tools to manage moods better.
Now let’s not forget about medication; some folks find relief from mood stabilizers or antidepressants under the care of their doctor.
It all comes down to understanding how these episodes affect your life and making sure you have the support system around you—whether that’s friends, family or professionals who get what you’re going through.
And remember: living with Bipolar Type 2 doesn’t mean defining yourself by it. With awareness and support, people lead very fulfilling lives despite this condition!
Understanding the Criteria for a Bipolar 2 Diagnosis: Key Insights and Information
Sure! Let’s talk about Bipolar 2 disorder and what it takes to get diagnosed. It can be a bit tricky, so hang tight while we break it down.
First things first, **Bipolar 2 disorder** isn’t just about mood swings. Sure, it has ups and downs, but the specifics matter a lot. The **DSM-5**, which is the manual mental health professionals use, lays out clear criteria for diagnosing it.
Here’s what you need to know:
- **Presence of Major Depressive Episodes:** You need to have had at least one major depressive episode. This isn’t just feeling sad for a few days. Think of it like a heavy cloud that doesn’t seem to lift for weeks or even months.
- **Hypomanic Episodes:** You also need to have experienced at least one hypomanic episode. This is like being on an emotional rollercoaster but without the full-on extremes of mania that you’d find in Bipolar 1. It can feel good at first—lots of energy, creativity, and maybe even some grand ideas—but it can turn into chaos.
- **No Full Manic Episodes:** One big thing: if you’ve ever had a full-blown manic episode (which is way more intense than hypomania), then you don’t fit the Bipolar 2 diagnosis. This is crucial because mania flips everything on its head.
- **Duration and Impact:** The depressive episodes often last for at least two weeks, while hypomanic episodes should last at least four days. Also, these mood changes gotta impact your life—like affecting your job or relationships—in a pretty significant way.
- **Not Better Explained by Another Condition:** Finally, mental health pros will check if your symptoms are better accounted for by another condition (like substance use or another psychiatric issue). If they are, then it’s not Bipolar 2.
Now here’s an important point: everyone experiences this differently. Some might feel really energized during those hypomanic phases; others may struggle with irritability or racing thoughts.
To connect on a human level here—imagine you’re going through life all bright-eyed during those high-energy moments but then suddenly crash hard into sadness that feels unshakable. It’s exhausting! A friend of mine went through this once; she talked about how she’d have bursts of creativity that felt magical only to be followed by weeks where getting out of bed felt impossible.
Understanding these criteria can help clarify things for those who think they might be experiencing similar patterns in their moods. Mental health isn’t straightforward; there are layers and nuances involved.
So remember: if you suspect something’s off with yourself or someone else regarding mood swings, talking to a mental health professional can really help sort through those feelings and find some clarity. Don’t hesitate to seek support!
Understanding Bipolar Disorders: Key Criteria for Differentiating Between Bipolar 1 and Bipolar 2
Bipolar disorders can be a bit tricky to navigate, especially when you’re trying to figure out the differences between Bipolar 1 and Bipolar 2. It’s essential to grasp the key features of each type, so let’s break it down in simple terms.
First off, Bipolar 1 Disorder is characterized by at least one full manic episode. This means that the person has experienced an elevated mood that lasts for at least one week, or even less if hospitalization is necessary. During this time, they might feel overly happy or irritable, and their energy levels can skyrocket.
Some symptoms of a manic episode include:
- Increased energy and activity
- Racing thoughts
- Decreased need for sleep
- Impulsive behaviors, like spending sprees or risky activities
Once I was talking to someone who had Bipolar 1. They shared how exhilarating it felt during those manic phases—like they could conquer anything! But afterward, the crash often left them feeling completely drained and depressed.
On the other hand, Bipolar 2 Disorder doesn’t involve full-blown manic episodes. Instead, it has what’s called hypomanic episodes. These are similar but less severe and don’t lead to significant issues in functioning or require hospitalization. Hypomania lasts for at least four days and might look like:
- Elevated mood with increased productivity
- Slightly decreased need for sleep but not too disruptive
- More talkative than usual or feeling full of ideas
- A tendency for risky behavior but usually not as extreme as in mania
Imagine feeling upbeat and creative without sliding into total chaos—that’s hypomania! It can sound really nice until depression hits hard later on.
Now, here’s a critical piece: both disorders may involve depressive episodes. For Bipolar 1, these can happen but aren’t required for diagnosis; however, with Bipolar 2, having at least one major depressive episode is crucial.
To wrap things up: Bipolar 1 features manic episodes that can be life-altering while Bipolar 2 has hypomanic episodes that are milder yet still impactful. Both types have depressive phases that warrant attention and care—making them serious conditions deserving proper support and treatment.
If you’re finding this all a bit confusing or know someone who struggles with these symptoms, reaching out to a mental health professional can make a world of difference! They can help clarify these experiences further and explore paths toward healing.
Alright, let’s talk about Bipolar II disorder. It can feel pretty overwhelming to dig into the criteria laid out in the DSM-5, but hang on; we’ll break it down a bit. First off, if you ever felt like you’re on an emotional rollercoaster, this might hit close to home.
So, Bipolar II is characterized by mood swings that aren’t just typical ups and downs. You’ve got major depressive episodes and at least one hypomanic episode. What’s hypomania? Well, think of it as a milder form of mania—you’re feeling super energetic and creative but without losing touch with reality.
I remember chatting with a friend who has Bipolar II; they described how during a hypomanic phase, it felt like everything clicked into place. They were writing poetry at 3 AM, feeling inspired and invincible. But then came the crash—a heavy depression that made getting out of bed feel like climbing Mount Everest.
Now, to meet the criteria for diagnosis: those depressive episodes can be pretty serious. We’re talking things like persistent sadness or irritability, loss of interest in activities you usually love (like binge-watching your fave show), trouble sleeping or sleeping way too much—and let’s not forget about that fun little side effect called guilt or worthlessness.
The thing is, this isn’t just about feeling sad or occasionally high-energy; it’s more intense than that. And those episodes need to cause significant distress or interference in your daily life—work, relationships, even just getting through a regular day.
One more thing—doctors look for these symptoms over a period of time and rule out other possible causes before landing on Bipolar II as the diagnosis. It’s tricky because people often mistake these moods for personality quirks or mood swings that we all experience sometimes.
So yeah, if you’ve ever felt caught between soaring highs and crushing lows without knowing where that rollercoaster might take you next? You’re definitely not alone in this journey. And understanding these criteria can be an important step towards finding hope—and possibly treatment.