You ever feel like your emotions are on a rollercoaster? Yeah, that’s pretty much what living with Bipolar II Disorder can be like. It’s like one minute you’re up—super creative, full of energy. Then the next, bam—you’re down in the dumps, struggling to even get out of bed.
A lot of folks don’t get it though. The ups and downs aren’t just part of life; they’re actually symptoms of a legit mental health condition. So let’s break it down together—what the DSM-5 says about Bipolar II, how it’s diagnosed, and why understanding all this matters. You with me? Cool! Let’s dive in.
Understanding the DSM-5 Criteria for Bipolar II Disorder: A Comprehensive Guide
Bipolar II disorder can be pretty tricky to wrap your head around, but understanding the DSM-5 criteria helps a lot. So, let’s break it down into digestible bits.
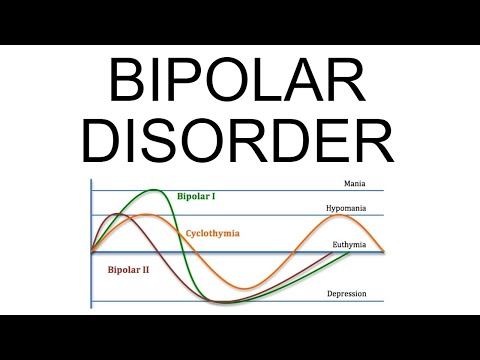
Bipolar II Disorder is characterized by mood swings that include episodes of depression and at least one hypomanic episode. It’s important to note that, unlike Bipolar I, individuals with Bipolar II don’t experience full-blown manic episodes. This distinction is crucial for diagnosis!
The DSM-5, or the Diagnostic and Statistical Manual of Mental Disorders, Fifth Edition, provides specific criteria for diagnosing Bipolar II disorder. Here’s how it works:
- Hypomanic Episodes: You need to have at least one hypomanic episode that lasts at least four days. Hypomania feels like an elevated mood but isn’t as intense as mania. You might feel super energized or unusually productive.
- Major Depressive Episodes: You also need to have a major depressive episode lasting at least two weeks. This can feel like a heavy weight on your shoulders—persistent sadness, fatigue, irritability, or loss of interest in things you usually enjoy.
- No Manic Episodes: The kicker here is that you can’t have had any manic episodes in your life. If you’ve had one of those wild episodes where you can’t sleep for days and feel invincible, then it’s not Bipolar II.
- Functional Impairment: These symptoms must cause significant distress or impairment in social or occupational areas of functioning. Basically, it interrupts your life in a noticeable way.
- Treatment Considerations: Often people with Bipolar II disorder may not recognize their hypomanic states since they can often feel good—so getting diagnosed might take time because folks often just think they’re being productive!
Now let’s talk about the emotional side a bit more because this stuff can get really personal! Imagine feeling on top of the world during your hypomanic phase: you’re crushing it at work, socializing like crazy, and feeling kind of invincible. But then when that wave crashes into severe depression? Ugh! It can make you feel like you’ve hit rock bottom after soaring so high.
Recognizing these patterns helps in understanding yourself better and working with professionals who know what they’re doing when it comes to diagnosing and treating mental health conditions.
So yeah, getting diagnosed with Bipolar II disorder isn’t just about ticks on a list—it’s about real experiences and emotions that affect day-to-day living. Understanding these criteria can help you navigate the ups and downs much more smoothly!
Understanding the Diagnosis of Bipolar II Disorder: Key Steps and Criteria
So, let’s chat about **Bipolar II Disorder**. It can sound kind of overwhelming, but breaking it down makes it easier to get a grip on what’s going on. Basically, it falls under the umbrella of mood disorders. You’ve got swings in mood that go from really high (that’s what they call hypomania) to pretty low (which is depression). But here’s the kicker: with Bipolar II, you never hit that full-blown mania they talk about in Bipolar I.
To wrap your head around this better, let’s look at some key **diagnostic criteria** from the DSM-5, which is basically the bible for mental health pros when diagnosing conditions:
1. Hypomanic Episodes: The person must have had at least one hypomanic episode lasting at least four consecutive days. This isn’t just feeling good; it has specific traits like increased energy or irritability.
2. Major Depressive Episodes: You also need to have experienced at least one major depressive episode. These episodes can be really tough—they last for two weeks or more and often involve feelings like sadness, fatigue, and loss of interest in activities that used to be enjoyable.
3. No Full Manic Episodes: Seriously! If you’ve ever had a full manic episode (like being up for days on end without sleep), you don’t fall into Bipolar II territory. So that’s an important distinction.
4. Mood Swings Are Disruptive: Your mood changes can’t just be a normal part of your personality; they need to seriously affect your daily life—like work or relationships.
Here’s something important: these episodes can happen pretty randomly or feel triggered by life events—maybe a breakup or losing a job might set things off. You know how some folks just seem more high-strung? Well, having Bipolar II might make those emotions hit harder for you.
And then you’ve got the whole “not being right” thing for some time before diagnosis too—that’s where intense feelings not only mess with your day but also feel like they come out of nowhere sometimes; it’s confusing!
Also worth mentioning is that depression here can sometimes look different than «textbook» sadness—it could rage, anxiety, or feeling super empty instead.
So after identifying these symptoms through self-reporting and sometimes family input (because friends and family often see stuff we might miss!), doctors usually do a thorough clinical interview and maybe some tests just to rule other stuff out—like substance abuse or other medical issues—since those can mimic bipolar symptoms as well.
Then there’s this part where professionals consider your **family history** because genetics can play a role in mental health stuff too! If someone else in your family has been diagnosed with a bipolar disorder or depression, it could give some clues.
Getting diagnosed isn’t easy-peasy and usually involves several conversations over time so doctors can see patterns rather than jumping to conclusions based on one bad day or week—trust me; it’s way more nuanced than that!
Finallyyy… if you’re thinking about getting evaluated, there’s no shame in asking for help; talking to someone who gets mental health is probably gonna help clear things up more than Googling answers ever would!
Just keep an open mind about what you might find out—it could lead you towards finding the right support and treatment options tailored specifically for *you*.
Comprehensive Guide to DSM-5 Bipolar II Disorder Criteria: Downloadable PDF Resource
Bipolar II Disorder can be pretty complex, but understanding its criteria in the DSM-5 is a crucial step in getting to grips with it. You know, the DSM-5 is like this big book of mental health diagnoses that professionals use. For Bipolar II, there are specific things they look for. Here’s a breakdown to keep it simple.
First off, **Bipolar II Disorder** involves two main types of mood episodes: **hypomanic episodes** and **depressive episodes**.
1. Hypomanic Episodes:
These are less severe than the manic episodes found in Bipolar I Disorder. People might feel really good, have lots of energy or just feel unusually productive without needing much sleep. But it’s not just about feeling great; there are some important *criteria*:
- It lasts at least four consecutive days.
- It includes three or more symptoms like increased self-esteem, decreased need for sleep, being more talkative than usual, racing thoughts, distractibility, and engaging in risky behaviors.
Imagine someone who suddenly feels energized and takes on multiple projects at work but doesn’t realize how their enthusiasm might annoy colleagues or lead to burnout later.
2. Depressive Episodes:
These can be pretty heavy and are often more recognizable than hypomanic ones. For an episode to count as part of Bipolar II:
- It should last at least two weeks.
- You’ll typically see five or more symptoms such as feelings of sadness or emptiness, loss of interest in activities once enjoyed, significant weight changes, fatigue or loss of energy, feelings of worthlessness or excessive guilt, difficulty concentrating.
Think about someone who used to love hanging out with friends but suddenly prefers staying home alone because everything feels overwhelming.
3. No Manic Episodes:
Here’s the catch—people with Bipolar II do not experience full-blown manic episodes that last for a week or longer (like what you’d see in Bipolar I). If these manic episodes do occur, then the diagnosis might change.
4. Impact on Life:
The symptoms should cause noticeable distress or impairment in social areas or other important functioning aspects like work or relationships. It’s not just about feeling down; it affects day-to-day living.
So if you’re piecing together whether someone fits this diagnosis based on the DSM-5 criteria, keep these points close by because they play a key role in understanding how Bipolar II impacts lives differently from other types.
In looking into all this stuff about Bipolar II disorder through the lens of mental health resources and guidelines helps individuals find their footing when navigating treatment options and support systems available out there! It’s essential—no one has to do this alone!
You know, bipolar II disorder kinda sneaks up on you. It’s like, one moment you’re feeling like you can conquer the world, and the next, you’re in this deep hole where getting out of bed feels like lifting a mountain. So, what’s really going on?
To break it down a bit, bipolar II is mostly about those ups and downs — but the ups are usually less intense than in bipolar I. It’s this thing called hypomania. You might feel energized, super creative, or even a bit impulsive. Now, that’d be awesome if it weren’t followed by these serious lows.
When diagnosing it, mental health pros look at some specific criteria from the DSM-5 (that’s the Diagnostic and Statistical Manual of Mental Disorders). Basically, they check if there have been at least one major depressive episode and at least one hypomanic episode in your life. But here’s the kicker: those hypomanic episodes can’t be severe enough to cause significant problems in your daily life or require hospitalization.
A friend of mine has had her struggles with this disorder. There were times she would joyfully paint for hours during her hypomanic phases, creating amazing artwork – paintings bursting with color and energy. But then came the crash: she’d feel worthless for weeks afterward. It’s such a roller coaster — exhilarating sometimes but also super exhausting.
And then there’s that element of time — it can drag on for years without diagnosis because it often gets masked as regular mood swings or stress-related stuff. Imagine someone telling you “just snap out of it” when a low point hits hard; that can be draining.
So basically, if you’re navigating these wild emotional highs and lows and think it might not just be regular mood swings? Talking to someone who gets all this can really help clear things up. It’s not just “in your head,” you know? There’s support out there for all of it — so hold onto hope!