You know that feeling when your body just seems to go haywire, but doctors can’t find anything physically wrong? Yeah, that’s somatoform disorder for you. It’s like your mind and body are having a miscommunication party, and you didn’t get the invite.
Imagine waking up with this nagging pain or fatigue. You go to the doc, and they run all these tests. Everything comes back normal. Yet, you feel awful. It’s confusing and frustrating, right?
This ain’t just in your head—well, sort of. Your emotions play a huge role in how your body reacts. That disconnect can lead to real symptoms: pain, nausea, whatever.
In this chat about somatoform disorder, we’ll untangle what it is and how it fits into the bigger picture of mental health. Are you ready? Let’s get into it!
Understanding Somatoform Disorder: Definition, Symptoms, and Treatment Options
So, let’s chat about somatoform disorder. This term might sound super clinical and confusing, but it’s basically about how our minds can influence our bodies in some pretty significant ways. To break it down, somatoform disorder involves physical symptoms that can’t be fully explained by medical conditions. It’s like your brain is playing tricks on your body, and you really feel those effects.
You might wonder how this all shows up in real life. Well, someone with a somatoform disorder might experience things like chronic pain, fatigue, or headaches—severe enough to interrupt their everyday life—yet all medical tests come back clear. It can be really frustrating! You want answers; you want to know why you’re feeling that way. But the truth? Sometimes the cause is more about what’s happening in your head than what’s going on physically.
Here are some common symptoms people might face:
- Chronic pain: Pain that feels very real but isn’t linked to an injury or illness.
- Fatigue: Constant tiredness that doesn’t improve with rest.
- Gastrointestinal issues: Such as nausea or even irritable bowel syndrome without any clear diagnosis.
- Numbness or tingling: Sensations that don’t have a medical cause.
- Anxiety or depression: Often runs alongside somatoform disorders since dealing with ongoing symptoms can take a toll emotionally.
It’s important to remember that these symptoms are real for the person experiencing them, even if doctors can’t pinpoint a physical issue. Imagine feeling super sick for weeks and then having doctors tell you there’s nothing wrong. That can mess with anyone’s head!
When it comes to treatment options, there are a few paths professionals may take:
- Therapy: Especially cognitive-behavioral therapy (CBT). This type helps people change negative thought patterns and cope more effectively with their symptoms.
- Psychoeducation: Just helping people understand what’s going on can provide relief and reduce anxiety around their symptoms.
- Medication: Sometimes prescribed for accompanying anxiety or depression but not for the somatic symptoms themselves as they may not respond to traditional treatments.
In essence, tackling somatoform disorder often requires a multi-pronged approach—addressing both psychological aspects and supporting the person’s overall mental well-being.
But what’s crucial is open communication between patients and healthcare providers. If someone has no clue why they’re feeling terrible day after day, they need support from professionals who truly listen and validate their pain. It’s frustrating when you feel unheard!
So yeah, if you find yourself or someone you care about struggling with similar issues, reaching out for help makes sense. Understanding this disorder is just as important as finding ways to treat it—not just because of the physical symptoms but because of the emotional journey wrapped around it all.
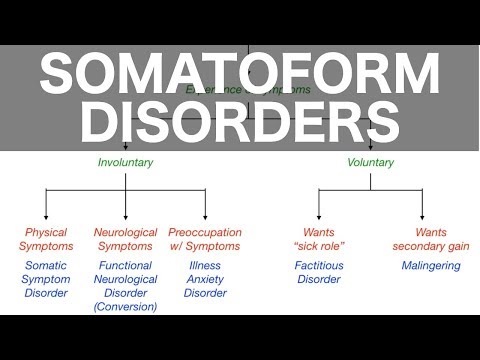
Understanding the Differences: Somatic Symptom Disorder vs. Illness Anxiety Disorder
So, let’s break down the differences between **Somatic Symptom Disorder** and **Illness Anxiety Disorder**. At first glance, they might seem similar, but there’s actually a pretty big distinction between the two.
Somatic Symptom Disorder is all about experiencing physical symptoms that cause you significant distress or impairment. The thing is, these symptoms don’t have to have a clear medical explanation. Maybe you feel pain in your chest or have stomach issues, and those feelings are very real to you. You might even see multiple doctors trying to find out what’s wrong, but nothing turns up.
On the other hand, with Illness Anxiety Disorder, it’s more about the fear of being sick rather than experiencing real physical symptoms. You might constantly worry that you have a serious illness based on minor signs or even just thinking about health issues in general. Like, maybe you read something online about headaches and suddenly believe you have a brain tumor—even though it’s just stress or lack of sleep causing those headaches.
It’s like when your friend feels tired after staying up late and thinks they must be coming down with something serious—just because they’re a bit run down! That constant worry? It defines Illness Anxiety Disorder.
Here are some key points to think about:
- Physical Symptoms: Somatic Symptom Disorder involves genuine physical symptoms that cause distress.
- No Clear Medical Cause: With Somatic Symptom Disorder, there’s often no identifiable medical issue behind the symptoms.
- Anxiety About Illness: Illness Anxiety Disorder centers around excessive worry about being gravely ill despite little to no symptoms.
- Focus on Symptoms vs. Fear: One focuses on actual experiences of pain (Somatic), while the other fixates on fearing illness (Illness Anxiety).
Sometimes people confuse these disorders for one another because they both relate to how our mind and body interact. But remember, if someone is genuinely feeling something physically painful, it doesn’t mean they’re faking it—it can deeply affect their life!
I remember hearing about a guy named Tom who felt intense stomach pain for months. He went through countless tests but found nothing alarming physically. Eventually, he learned he had Somatic Symptom Disorder and went into therapy to address his underlying anxiety and stress related to his symptoms. It was eye-opening for him—realizing his mind was influencing how his body felt!
Just keep in mind that both of these disorders are valid experiences that deserve compassion and understanding from everyone around them. So if you’re feeling overwhelmed by worries about your health—or if you’re dealing with unexplained aches—it might be worth talking to someone who understands this stuff better!
Understanding Somatic Symptom Disorder: A Comprehensive Guide to DSM-5 Criteria and Treatment
So, let’s chat about somatic symptom disorder, or SSD for short. It sounds intense, but really it’s about how our minds and bodies can be super connected. Sometimes when we’re feeling stressed or anxious, we can have physical symptoms that feel very real. You know? Like headaches or stomachaches that just won’t quit.
What’s the deal with SSD? Well, in the DSM-5—the big book of mental health diagnoses—they’ve laid out some criteria to help professionals figure this out. Basically, SSD is diagnosed when you have one or more physical symptoms that cause significant distress or problems in your life. This isn’t just a case of “Oh, I have a headache.” We’re talking about stuff that interferes with daily activities.
To break it down further:
- You’ve got one or more somatic symptoms (like pain or fatigue).
- You have excessive thoughts about these symptoms—like you worry way too much about what they mean.
- Your feelings are causing major anxiety and impact your social life, work, and daily activities.
It’s not just in your head—it’s a real experience! But what makes SSD tricky is that you might see doctors over and over without any clear medical cause for those symptoms.
Now here’s where it gets interesting. Sometimes people jump to conclusions about SSD being all in your head. But hold on! The thing is they can feel real physically and emotionally. Think back to when a friend had a rough week at work; they ended up with severe stomach pain but couldn’t find anything wrong physically. That could be something like SSD at play!
Treatment options are essential too. Therapists often work with cognitive-behavioral therapy (CBT) to help change those worry patterns into something more positive. Seriously though, CBT can guide you on how to cope better and even lessen the impact those pesky symptoms have on your life.
And here’s a little nugget of reality—sometimes medication is suggested if there’s also anxiety or depression tagging along for the ride. That doesn’t mean it’s all magic pills; it’s just another tool in the toolbox, so to speak.
So if you’re ever feeling like your body is acting out because of stress or emotions when nothing seems medically off? It might be worth chatting with someone who gets it, because understanding somatic symptom disorder could really change how you view those experiences!
Somatoform disorder can be a bit tricky, you know? It’s one of those things that people often don’t understand. So, let’s break it down together.
Imagine someone who’s feeling really, really unwell but, when they go to the doctor, nothing seems to show up on any tests. Like, there could be pain or fatigue or even weird sensations in their body. It’s real for them, but there are no physical explanations. That’s where somatoform disorder fits in. It’s when emotional distress manifests itself through physical symptoms. You’re not faking it; it just is what it is.
I remember this friend of mine. She started having horrible stomach aches every time she thought about work. I mean, we all have those days when the job feels too much, right? But for her, it turned into this chronic issue that kept her from doing stuff she loved. After a lot of back and forth with doctors and no answers, we finally realized that her anxiety was affecting her body in ways she didn’t even see coming.
This kind of disorder makes it hard to separate what’s happening mentally from what feels physically real. And that can lead to frustration—both for the person experiencing it and their loved ones. You want to help them feel better! But sometimes they might need more understanding rather than just “It’s all in your head.” Because honestly? What does that even mean?
In mental health contexts, addressing somatoform disorder can take a bit more finesse than simply treating physical symptoms with meds or tests. Therapy can be a game-changer here—helping individuals navigate their feelings and discover how stress might play into their physical experiences.
The big takeaway? Our minds and bodies are more connected than most of us realize. Staying aware of that connection can open up pathways to healing that go beyond surface-level symptoms. So next time someone mentions strange pain or discomfort with no clear source, maybe just remember: there could be so much more beneath the surface waiting to be understood and addressed with care and compassion.