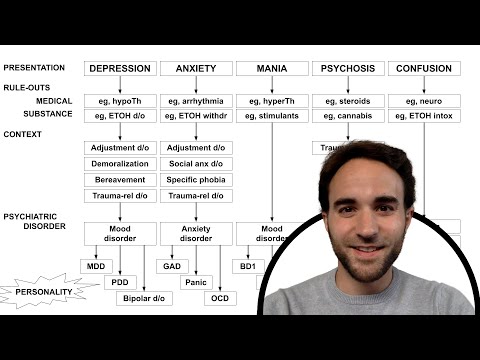
Hey, you! Let’s chat about something that sounds super technical but is actually really important. I’m talking about differential diagnosis in the DSM-5. Sounds a bit dry, huh? But stick with me.
Imagine you’re going to the doctor. You tell them you feel awful but can’t quite pin down why. They run tests and ask questions, trying to figure out what’s going on. That’s basically what mental health pros do with this whole differential diagnosis thing.
It’s about identifying what’s really happening beneath the surface when it comes to mental health conditions. And trust me, it gets pretty fascinating once you dig in! Being able to tell one condition from another can change someone’s life for the better.
So, whether you’re a pro or just curious about mental health stuff, let’s break this down together in a way that feels simple and relatable. Sound good?
Understanding Differential Diagnoses in Mental Health: A Comprehensive Guide
So, let’s chat a bit about differential diagnoses in mental health. It’s one of those things that might sound super complicated at first, but stick with me and it’ll all make sense. Basically, differential diagnosis is a fancy term for figuring out what mental health condition someone has by comparing their symptoms to other possible conditions.
When you walk into a therapist’s office or a psychiatrist’s clinic, you’re not just seeing them to get a quick fix. They really need to dissect what’s going on with you—like the last puzzle piece in a jigsaw that can change the whole picture. This is where differential diagnosis comes into play.
First off, why is it so important? Well, different mental health issues can look pretty similar on the surface. Take depression and anxiety, for example. They can share symptoms like trouble sleeping or feeling restless. If a clinician jumps in too quickly and says “Aha! It’s depression!” without considering other possibilities, they could miss something crucial.
Now, let’s break down how this works:
- Clinical Observation: This starts with understanding your history and what you’re feeling right now. A skilled clinician will listen carefully to your story and observe your behavior.
- Symptom Checklists: Sometimes they’ll use standard questionnaires or criteria found in tools like the DSM-5 (Diagnostic and Statistical Manual of Mental Disorders). It helps them compare your symptoms against established categories.
- Rule Out Medical Issues: Physical problems can masquerade as mental health conditions. For example, hypothyroidism can resemble depression, so they may check for medical reasons before jumping straight into a mental health label.
This process is really about asking questions—lots of questions! Just think about how detectives work; they gather clues before making an arrest.
Example: Let’s say someone walks in saying they’re feeling really low and have lost interest in things they used to enjoy. The therapist might first consider major depressive disorder but could also think about possible bipolar disorder if there are hints of mood swings we don’t know yet.
It’s also essential to understand that some conditions can coexist. Imagine having anxiety while dealing with chronic pain or depression showing up alongside PTSD—those complexities make this process even more vital.
As part of this journey, clinicians also look at duration and impact on your daily life. Just because you’re feeling sad one week doesn’t mean you’ve got clinical depression; it might be situational or due to stress.
Another vital point? Always be open during these conversations! If you’re willing to share honestly about your experiences—including those messy emotions—it’ll help your therapist box things up correctly. And hey! If they get it wrong? You don’t always have to accept it blindly; feel free to ask questions or seek a second opinion.
In short, understanding this whole differential diagnosis thing is key because it paves the way for tailored treatment options that fit *you* best—because let’s face it; no two people are exactly alike! So if you’re stepping into therapy soon or have been thinking about it, know that this complicated sounding stuff is just part of ensuring you get the care that’s right for you!
Understanding Differential Diagnosis in the DSM: A Key to Accurate Mental Health Assessment
Alright, so let’s break down differential diagnosis. You might be asking, what the heck is that? Well, it’s basically a way for mental health professionals to figure out which mental health condition someone has when they have symptoms that might fit more than one diagnosis. It’s kind of like being a detective—really! Instead of jumping to conclusions right away, they need to gather clues and rule things in or out.
Now, when you’re looking at the DSM-5, or the Diagnostic and Statistical Manual of Mental Disorders, it’s your go-to for understanding these various mental health conditions. The DSM lists symptoms and criteria for different disorders. But here’s the catch: many disorders can share similar symptoms. So, how do you differentiate?
- Collecting Symptoms: First things first: your therapist will ask a ton of questions about how you’re feeling. Are you anxious? Depressed? It’s all about gathering info. For instance, if you’re feeling really low but also super anxious, it could point to either major depression or an anxiety disorder.
- Time Frame: Another thing they consider is how long you’ve been experiencing those symptoms. If it’s been a few weeks versus several months, it can steer them toward one diagnosis over another.
- Cultural Context: Cultural factors play a big role too! What’s normal in one culture might not be in another. If you’re coming from a background where emotional expressions are different—maybe you’re more stoic—it could influence how your symptoms are interpreted.
- Physical Health: Sometimes physical issues can mimic mental health problems. For example, thyroid problems might make you feel depressed or anxious. That’s why tests like blood work can rule out medical causes before settling on a mental health diagnosis.
The thing is, differential diagnosis isn’t just some technical term; it really impacts how effective treatment will be. When professionals correctly identify what someone is facing, they can tailor their interventions better—like if you’re diagnosed with generalized anxiety disorder instead of social anxiety disorder. One may need cognitive-behavioral therapy focusing on different aspects than the other!
This process isn’t always quick or easy; it takes time and sometimes multiple visits before everything clicks together perfectly. Here’s an example: imagine someone showing signs of depression but later realizes they’ve got ADHD instead. They might just need help managing their focus rather than just working on their mood!
You see, accurate assessment through differential diagnosis is super vital in getting the right support for whatever you’re dealing with emotionally or mentally! The better the understanding of what’s really happening inside your head (or heart), the better equipped everyone is to help you feel like yourself again.
Understanding the DSM-V: Key Insights and Resources for Mental Health Professionals
Understanding the DSM-5 is crucial for anyone involved in mental health. It stands for the Diagnostic and Statistical Manual of Mental Disorders, Fifth Edition. So, basically, it’s like a big book where mental health professionals can find guidelines to help diagnose mental health conditions.
The DSM-5 helps create a common language for clinicians. This consistency is important so that everyone—doctors, therapists, and even researchers—can communicate clearly about mental health issues. Imagine trying to discuss something really complex but using different words; it would get confusing fast, right?
Now let’s talk about differential diagnosis. This is where it gets interesting. Differential diagnosis means sorting through symptoms to identify which specific disorder a person might have. Symptoms can overlap between disorders, making this part tricky.
When making these distinctions, professionals often rely on listing key symptoms:
- Nature of Symptoms: What exactly are they experiencing? Is it sadness or exhaustion? These little details matter.
- Duration: How long have these symptoms been present? Something short-term may not be the same as something chronic.
- Cultural Context: Cultural factors can influence how symptoms present themselves or how they’re perceived.
For instance, let’s say someone walks into therapy feeling extremely anxious and restless. On one hand, this could hint at Generalized Anxiety Disorder (GAD). But on another hand—if they’ve also experienced traumatic events—might it point toward PTSD instead? Here’s where differential diagnosis comes in handy.
A key resource within the DSM-5 is the “Cultural Formulation Interview.” This tool allows clinicians to understand cultural dimensions that might affect a patient’s experience and expression of distress. It’s all about recognizing that one-size-fits-all doesn’t always apply in mental health.
Another thing to know is that the DSM-5 encourages a dimensional approach alongside categorical diagnoses. Instead of just checking boxes based on yes/no answers, many conditions are evaluated on a scale from mild to severe. So if you’re dealing with depression, for example, you’ll want to assess how deeply it’s impacting daily life.
It’s also worth mentioning comorbidity; this term refers to when someone has two or more disorders at once. This complicates differential diagnosis significantly! A patient might have both anxiety and depression simultaneously—not uncommon at all—and teasing apart which symptom belongs where can be a real puzzle.
One final note—you can’t rely solely on the DSM-5 for good practice in psychology or psychiatry. It should serve as a guide but not your only resource. Clinical judgment and patient context are essential too.
In sum, understanding the DSM-5 isn’t just knowing what each disorder entails; it’s about seeing the bigger picture of someone’s life experiences and providing them with tailored support based on those insights.
Differential diagnosis can feel like navigating a maze for mental health pros. You know, it’s when you figure out which mental health issue someone is facing by ruling out other possibilities. It’s kinda like being a detective, piecing together clues to get to the heart of what’s going on.
The DSM-5, which stands for the Diagnostic and Statistical Manual of Mental Disorders, is like this huge reference book used by therapists and psychiatrists. It’s packed with lists of symptoms for tons of mental health conditions. But here’s the thing—just because someone has certain symptoms doesn’t mean you can slap a label on them right away. It’s not that straightforward.
I remember a time when a friend was feeling super anxious all the time and thought they might have Generalized Anxiety Disorder (GAD). They were worried about everything: school, relationships, even if there was enough coffee at home! But after talking to a therapist, it turned out their anxiety was more about underlying issues from past trauma rather than GAD itself. That moment really showed me how important it is to look deeper before making a diagnosis.
So, basically, differential diagnosis requires considering all sorts of factors—like medical history, current stressors, and even personality traits. A good therapist knows that two people can show similar symptoms but be dealing with totally different things underneath. And being thorough in this process can really make or break treatment options.
It’s also crucial because misdiagnosis can lead to inappropriate treatments—a person suffering from depression might end up on meds that don’t help if they’re actually experiencing something else entirely! That would be frustrating for anyone seeking help.
To sum it up? Differential diagnosis in the DSM-5 isn’t just checking boxes. It requires diving deep into each individual’s story. Giving them the right label means giving them the best shot at healing—so yeah, it’s worth taking the time to really listen and explore those layers.