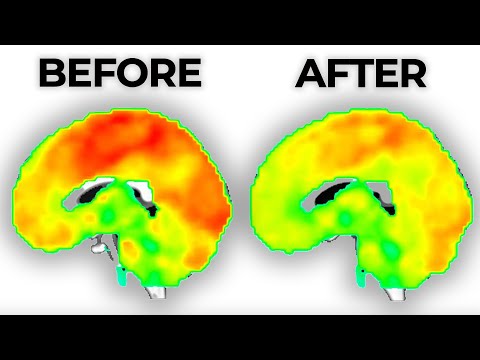
You know, we all hear about antidepressants and how they can help people feel better. But what about the long-term effects on your brain?
Seriously, it’s a big deal. I mean, these pills are prescribed like candy sometimes, right? So, what’s really going on up there after years of taking them?
That’s the thing—everyone’s different. Some folks swear by them, while others have questions. It gets pretty complex when you dig in.
Let’s chat about how these meds can change your brain over time. You might be surprised at what we find out together!
Exploring the Long-Term Effects of Antidepressants on Brain Function and Mental Health
Antidepressants can be a real lifeline for many people battling depression and anxiety, but there’s a lot to unpack when it comes to their long-term effects on brain function and mental health. Let’s break it down.
First off, the brain is super complex. It relies on neurotransmitters like serotonin and dopamine to regulate mood. Antidepressants primarily target these chemicals, helping to balance them out. But here’s the thing: long-term use may change how your brain operates, sometimes in ways we don’t fully understand yet.
1. Neuroplasticity
One cool aspect of the brain is neuroplasticity. This means your brain can adapt and change over time. Some studies suggest that long-term antidepressant use might actually enhance neuroplasticity. This could help with learning and memory—so that’s a plus! Still, other research hints at potential downsides, like changes in how you respond to stress.
2. Dependence vs. Withdrawal
It can be tricky when you’ve been on antidepressants for a while. Some folks might find they develop what feels like dependence on them—basically, their brains get used to the medication being there, which can complicate things if they decide to stop taking it. Quitting suddenly can lead to withdrawal symptoms that are uncomfortable, so tapering off under a doctor’s supervision is usually recommended.
3. Emotional Blunting
Another thing you’ve probably heard about is emotional blunting. This means some people report feeling dulled emotions or not experiencing highs and lows like they used to while taking antidepressants long-term. It might help with anxiety or depression but could also take away some joy or excitement about life—you know?
4. Impact on Other Medications
If you’re thinking about combining antidepressants with other medications or therapies, make sure you’re in touch with your healthcare provider regularly. Sometimes, long-term antidepressant use can interact with other treatments in unexpected ways.
5. Not for Everyone
Remember that not everyone experiences these effects the same way! For some folks, antidepressants are truly life-changing and improve overall well-being without causing major issues down the line.
Let me share a quick story: My friend Lisa struggled with severe anxiety for years before starting an SSRI (a common type of antidepressant). At first, it was like night and day—the relief she felt was immense! But after about two years, she noticed she couldn’t quite feel happiness the way she once did; it scared her a bit because she loved laughing freely with friends again.
In essence, while antidepressants can be incredibly helpful, it’s crucial to understand how they may impact your brain over time—both positively and negatively. Always keep an open line of communication with your doctor about any changes you notice along the way—because mental health is all about finding what works best for you!
Exploring the Connection: Can Lexapro Cause Joint Pain?
Lexapro, or escitalopram, is a popular antidepressant that belongs to the selective serotonin reuptake inhibitors (SSRIs) class. It’s often prescribed for conditions like depression and anxiety. But, like any medication, it can come with some side effects, and you might be wondering about its connection to joint pain.
First off, joint pain is not exactly a common side effect of Lexapro. Most people take it without any issues related to their joints. However, everyone’s body reacts differently to medications. Some folks do report experiencing joint discomfort after starting Lexapro or increasing their dosage.
Now, let’s dig into the science a bit. The thing is, SSRIs can affect your body in various ways. They influence serotonin levels—this brain chemical that plays a big role in mood regulation but also impacts other bodily functions. Serotonin affects various systems in your body, including those that regulate inflammation and pain sensation. So there’s a chance that if the medication messes with your serotonin balance, it could lead to some unexpected aches and pains.
Moreover, some individuals might develop an allergic reaction to Lexapro. This isn’t super common but can manifest as joint pain or swelling among other symptoms. If you suddenly notice discomfort after starting the med, it’s worth mentioning to your doctor.
Another factor could be changes in activity levels. When people start feeling better on antidepressants like Lexapro, they often become more active again after a period of feeling low energy or unmotivated due to depression. This sudden increase in physical activity could lead to sore joints simply because your body isn’t used to it yet!
But here’s something else: long-term use of certain medications can lead to muscle stiffness. While this isn’t necessarily joint pain per se, muscle issues can cause you to feel discomfort around the joints too.
If you’re ever facing unexplained joint pain while on Lexapro—or any medication for that matter—it’s super important not to just brush it off or self-diagnose. Seriously! You should have a convo with your healthcare provider about what you’re feeling so they can help you figure out if it’s related or just coincidental.
In summary:
- Joint pain isn’t common with Lexapro: Many people take it without issues.
- Serotonin effects: It may influence inflammation and pain sensations.
- Allergic reactions: Can occur in rare cases.
- Lifestyle changes: Increased activity might lead to soreness.
- Muscule stiffness: Long-term use could contribute indirectly.
Ultimately, staying aware of how you feel while on medication is key! And if something seems off? Just reach out for help—you don’t have to navigate this alone!
Understanding the Link Between Antidepressants and Constipation: What You Need to Know
When we talk about antidepressants, most people think about their impact on mood, right? But here’s the thing – they can also mess with your gut. Yeah, seriously. One common issue is **constipation**. Let’s break this down.
How Antidepressants Work
Antidepressants mainly target neurotransmitters in the brain, like serotonin and norepinephrine. These chemicals help regulate mood but also play a role in other bodily functions, including digestion. So when you tweak these systems, it’s no surprise that your digestive system might get a little out of whack.
Why Constipation Happens
A lot of antidepressants can slow down gut motility – basically how fast food moves through your intestines. This is often due to increased serotonin levels in the gut. It might sound like a good thing for your mood, but it can lead to **sluggish** digestion.
Different Types of Antidepressants
Not all antidepressants cause constipation equally. Here’s a quick look:
- SSRIs (Selective Serotonin Reuptake Inhibitors): These are the most commonly prescribed ones—think fluoxetine or sertraline. While they help with depression, they can relax muscles in your gut too much.
- SNRIs (Serotonin-Norepinephrine Reuptake Inhibitors): Medications like venlafaxine can also contribute to constipation issues due to their dual action on serotonin and norepinephrine.
- TCA (Tricyclic Antidepressants): These older meds are notorious for causing constipation since they block certain receptors that affect motility.
- Other medications: Some atypical antidepressants may have side effects that lead to gastrointestinal problems as well.
Real-World Example
Let’s say you start taking an SSRI for depression and notice your stomach feels heavy and you’re not going as often as before. You might think it’s just your diet or stress—but it could be linked to the medication itself.
What You Can Do
If you’re facing constipation from antidepressants, don’t just suffer in silence! Talk to your healthcare provider about it. They might recommend dietary changes or even consider adjusting your medication.
- Fiber Intake: Increasing fiber in your diet can help get things moving again.
- Stay Hydrated: Drink plenty of water; hydration plays a crucial role in digestion.
- Physical Activity: Regular exercises like walking or yoga can stimulate bowel movements too.
The Bottom Line
Understanding the link between antidepressants and **constipation** isn’t just about comfort—it matters for overall health too! You want your body feeling good while managing mental health issues effectively.
So if you find yourself stuck in this situation, remember: it’s important to reach out for help so you don’t have to deal with these uncomfortable side effects alone!
You know, talking about antidepressants can feel a bit heavy sometimes. I mean, they’re a lifeline for many, but the whole long-term effect thing? It’s complicated. The debate around it can get pretty intense, and that’s just life in the mental health world.
So, let’s say you’ve been on antidepressants for a while. Maybe you started them during a tough phase – like when everything felt gray and endless. I remember chatting with a friend of mine who went through a really rough patch. She found herself feeling numb at one point, and while those meds helped lift her out of that dark place, she started to wonder about what might be going on in her brain after years of use.
Antidepressants can change how your brain works over time. They tweak the balance of neurotransmitters—those little guys like serotonin and dopamine that play major roles in mood regulation. But what happens after years? Some studies suggest there might be some alterations in brain structure or function—you know, stuff like neuroplasticity (fancy word alert!) which is how our brain adapts to experiences over time.
That said, it’s not all doom and gloom! For many people, the benefits outweigh potential risks. After all, if medication helps you feel more like yourself again and get back into life—working or enjoying time with friends—that’s super valuable. And here’s the thing: everyone’s different. Your experience can look totally different from someone else’s.
But maybe you’re wondering about how these meds could impact you down the line? Some folks have reported withdrawal symptoms when they stop taking them suddenly or even challenges with depression resurfacing later on. It’s totally understandable to have concerns. The good news is that if you’re feeling uneasy about your medication or its effects, that convo with your doctor is so important.
At the end of the day, understanding our mental health journey means balancing the pros and cons—and sometimes unearthing more questions than answers. It’s messy but also kind of beautiful in its way; it’s about finding what works best for us as individuals while keeping ourselves informed along the way!