So, you know when your body feels off but doctors can’t find anything wrong? Yeah, that’s a real thing. It’s called somatoform disorder. Sounds heavy, right?
But it’s more common than you think. You might even know someone dealing with it. It can feel pretty confusing and frustrating for both the person going through it and their loved ones. Like, how do you explain something that seems all in your head but feels so real?
Let’s talk about what this actually looks like. We’ll dig into the emotional side of it, the struggles people face, and maybe even shine a light on some paths to understanding. Buckle up; it’s a journey worth taking!
Understanding Somatic Symptom and Related Disorders: Insights into Mind-Body Connections
Understanding Somatic Symptom and Related Disorders is all about recognizing how our minds and bodies are connected, which can sometimes lead to confusing situations. If you’ve ever felt pain or discomfort that just doesn’t seem to have a clear physical cause, you might be touching on this realm.
So, let’s break it down a bit. Somatic Symptom and Related Disorders (SSRD) are conditions where you experience physical symptoms that can’t be fully explained by medical issues. Your mind plays a huge role here; stress, anxiety, and past experiences can manifest in your body in ways you might not expect.
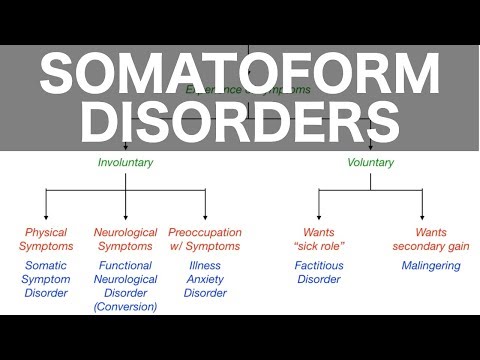
- Somatic Symptom Disorder: This involves having one or more distressing symptoms that disrupt your daily life. For instance, someone might experience chronic pain without an identifiable cause, but the suffering is very real.
- Illness Anxiety Disorder: Here, a person is preoccupied with the fear of having or developing a serious illness. You know that friend who thinks every little headache means something dire? That’s kind of what’s going on.
- Conversion Disorder: This is when psychological stress manifests as physical symptoms like paralysis or non-epileptic seizures. Imagine being completely unable to walk after a significant emotional trauma—it’s baffling but also so real.
It’s like your brain pulls some sneaky tricks on your body! Let me share an example. Picture Sarah, who loses her ability to speak after going through a really painful breakup. The doctors find nothing physically wrong with her vocal cords. But for Sarah, the silence is deafening and absolutely painful—the mind-body connection couldn’t be clearer.
So why does this happen? Well, sometimes emotions can be tricky to deal with head-on. When they get bottled up, they might show up as physical complaints instead of feelings—like anxiety manifesting as stomachaches or headaches.
Treatment for these disorders usually involves addressing both the physical and psychological aspects of the situation simultaneously; it’s not just about treating symptoms but really getting into what’s going on beneath the surface.
Therapies like Cognitive Behavioral Therapy (CBT) can help by changing negative thought patterns and teaching coping strategies for managing stress and emotional pain more effectively.
In addition, medication may also play a role in treatment—especially if anxiety or depression is involved—but that needs careful consideration from healthcare providers because it varies from person to person.
While SSRDs can feel intimidating or strange because they blur the lines between mind and body, understanding them opens doors for compassion—for yourself or others dealing with these disorders. Remember that no symptom is too small to discuss with someone who understands how deep this connection goes—it could lead to relief in ways you hadn’t expected!
Understanding Somatic Symptom Disorder: Insights from the DSM-5
Understanding Somatic Symptom Disorder can be a bit of a journey. The DSM-5, which stands for the Diagnostic and Statistical Manual of Mental Disorders, is basically the big book of mental health diagnoses. It helps professionals understand and categorize different mental health conditions, including somatic symptom disorder (SSD).
What is Somatic Symptom Disorder? Well, it’s when someone has physical symptoms that cause distress or impairment in daily life. These symptoms are real to the person experiencing them, even if medical tests don’t find anything wrong. Imagine feeling constant pain in your back or fatigue that just won’t go away. You visit doctors, but they can’t find a physical cause. That can be super frustrating!
One important thing to note is that with SSD, it’s not just about having physical symptoms; it’s also about how you feel about those symptoms. A person might worry excessively and get really anxious about what those symptoms could mean. Basically, the emotional response plays a significant role here.
Diagnostic Criteria in DSM-5 outlines what qualifies as SSD. It includes:
- You have one or more symptoms that are distressing or disrupt your life.
- You have excessive thoughts, feelings, or behaviors related to these symptoms.
- The symptoms persist for more than six months.
So why does this happen? Well, there isn’t always a clear answer. Stress and trauma can contribute massively to developing SSD. For instance, if someone has had a rough childhood or went through something traumatic, their body might react by manifesting these physical sensations as a way of coping with emotional pain.
Now let’s chat about treatment. There isn’t a one-size-fits-all approach here; often it involves therapy like Cognitive Behavioral Therapy (CBT). This type of therapy helps change negative patterns of thinking and behavior that can make the symptoms worse. Plus, sometimes medication is prescribed to help with anxiety or depression if they’re part of the picture.
It can get really complex when talking about somatoform disorders since they overlap with other issues like anxiety disorders and depression too! So navigating through this isn’t easy; progress might feel slow at times.
But here’s where some hope comes in: many people with SSD do respond well to treatment over time! If you’re feeling trapped by these frustrating symptoms or know someone who is, connecting them with professional help could be a game changer.
Remember: you’re not alone in this—there’s understanding out there and ways to cope with what you’re going through!
Understanding Somatoform Disorders: Key Examples and Insights
Somatoform Disorders can be pretty confusing, both for those experiencing them and for the people around them. So, let’s break it down in a way that makes sense. Essentially, these disorders involve physical symptoms that can’t be fully explained by medical conditions. It’s like your brain is sending signals to your body that create real discomfort or pain, but there’s no actual injury or illness going on.
You know how sometimes when you’re stressed, you might get a headache or feel sick to your stomach? That’s kind of a small example of how our emotions can impact our physical well-being. But with somatoform disorders, it goes way deeper than just the occasional stress headache.
- Somatic Symptom Disorder: This is when someone has persistent physical symptoms that cause significant distress or problems in daily life. Imagine constantly feeling pain but no doctor can pinpoint why.
- Illness Anxiety Disorder: Here, a person worries excessively about having a serious illness, even if there are no significant symptoms. It’s like being convinced you’ve got something really bad simply because you read about it online.
- Conversion Disorder: This one involves neurological symptoms like paralysis or seizures without a medical explanation. Think about someone suddenly unable to move an arm after experiencing a traumatic event—it’s real to them but doesn’t have an underlying cause.
So why does this happen? Well, the mind and body are super connected. You could be dealing with unresolved trauma, anxiety, or depression that manifests physically. For instance, I remember a friend of mine who developed mysterious back pain right after going through a tough breakup. She wasn’t aware of how much emotional weight she was carrying until her body started acting out.
Living with these disorders can be tough. It often leads people on an exhausting journey through various doctors’ offices because they genuinely feel unwell yet get told everything looks fine! That disconnect can lead to frustration and feelings of being misunderstood.
Treatment often involves therapy—particularly cognitive behavioral therapy (CBT)—which helps reframe the thought patterns associated with the physical symptoms. Sometimes medications might be used to help manage anxiety or depression too; but it’s not just about masking the symptoms; it’s about addressing what’s going on emotionally.
In short, somatoform disorders illustrate how intertwined our mental state and physical sensations are. Understanding this connection could make all the difference in finding the right support and getting better!
So, somatoform disorders, huh? It’s a pretty confusing topic, and honestly, it can feel like a maze trying to understand them. Basically, these disorders involve physical symptoms that don’t really have an underlying medical cause. Instead of being about the body itself, it’s more about the mind—like when emotions manifest as physical pain or discomfort.
I remember a friend of mine named Lisa. She’d always complain about severe headaches and stomach aches but every time she went to the doctor, they’d run tests and find nothing wrong. It was so frustrating for her because she was genuinely in pain but couldn’t get a clear answer. People around her often thought she just wanted attention or was being dramatic. But what they didn’t see was her struggle; the constant cycle of seeing doctors only to be told it’s “all in your head.”
The thing is, our minds are super powerful. Stress and anxiety can cause all sorts of crazy stuff to happen in our bodies. It’s like when you’re nervous before a big presentation—your stomach might churn or your palms might sweat. For some folks with somatoform disorders, this relationship gets tangled up in a way that results in persistent symptoms that can feel very real.
Treatment often involves therapy rather than medication alone. Cognitive-behavioral therapy (CBT) has been shown to help people change their thought patterns and coping mechanisms, which makes sense because addressing those underlying emotional issues can lead to some seriously positive changes physically too.
But navigating this whole situation isn’t easy for anyone involved—the person experiencing it or their family and friends who are trying to support them. There can be misunderstandings that make things harder; think about how Lisa felt when people dismissed her pain as fake. It’s so important for those around someone with these kinds of challenges to approach things with empathy.
So you see? It’s complex! But at the end of the day, understanding that emotions can have real physical consequences is key in breaking through this maze of somatoform disorders. It’s all about connecting the dots between mind and body—because they’re not so separate after all!