So, let’s chat about SSRIs and anxiety for a sec. You know, those little pills that people pop when they’re feeling super anxious?
It’s kinda wild, right? On one hand, they’ve been a lifesaver for so many. But on the other hand, it’s not always clear-cut. Some folks even find themselves feeling more anxious after starting them. Like, what gives?
You might be thinking, “Wait, aren’t these supposed to help?” Seriously, it’s one of those things that doesn’t get talked about enough in mental health circles.
So buckle up! We’re gonna dig into this paradox together and see what’s really going on.
Understanding the Paradoxical Effects of SSRIs: Why Some Experience Increased Anxiety
SSRIs and Anxiety, it’s a topic that brings up a lot of questions, right? Selective serotonin reuptake inhibitors (SSRIs) are often prescribed for depression and anxiety disorders. But here’s where things get interesting: not everyone feels better. Some people end up feeling even more anxious when they start taking these medications. What gives?
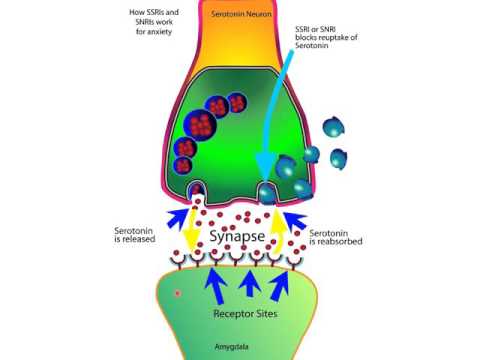
So, let’s break down why this happens. First off, SSRIs work by increasing the levels of serotonin in the brain, which is like a chemical messenger that helps regulate mood. You know? It seems logical that more serotonin should mean less anxiety. But it’s not always that straightforward.
One possible reason for increased anxiety is related to how long it takes for SSRIs to really kick in. When you start taking them, it can take several weeks before you notice any changes in your mood or anxiety levels. And during that waiting period, those initial side effects can be tough to handle.
Another thing is the body’s adjustment process. Your brain doesn’t like sudden changes, so when you introduce SSRIs into your system, it might react with heightened anxiety as it tries to find balance again. Kind of like your body throwing a mini tantrum while getting used to the new routine!
Also, it’s worth considering individual differences in biochemistry. Seriously! Everyone’s brain is wired differently. Some folks might not respond well to SSRIs because their specific type of anxiety or depression doesn’t jive with how the medication works.
There’s also this concept called anxiety sensitivity. It’s basically when someone has an exaggerated fear of physical sensations associated with anxiety (like a racing heart or sweating). When SSRIs first alter these sensations—by changing serotonin levels—it can sometimes make things feel worse before they get better.
Lastly, some people may misinterpret their symptoms during SSRI treatment. If you’re used to feeling down and suddenly you’re just feeling nervous without that sad blanket over you? That shift can feel pretty overwhelming at first.
In short:
- Adjustment Period: Initial side effects may lead to increased anxiety.
- Body’s Reaction: Your brain might resist sudden changes.
- Individual Responses: Personal brain chemistry plays a large role.
- Anxiety Sensitivity: Misinterpretation of physical symptoms can add stress.
So yeah, if you or someone you know experiences increased anxiety with SSRIs, it’s not uncommon at all! It could be part of the process—or something more individualistic going on with brain chemistry. Just remember: patience is key! Talking openly with a healthcare provider about these feelings can help adjust treatment as needed without going through unnecessary stress alone.
Is Long-Term Use of Lexapro Safe? Exploring the Considerations for Staying on Antidepressants
Is Long-Term Use of Lexapro Safe? This is a question that often pops up for folks who are considering or currently on this medication. Lexapro, or escitalopram, is a popular SSRI (selective serotonin reuptake inhibitor) that’s commonly prescribed for depression and anxiety. Many people find it effective, but the debate around long-term use is ongoing. Let’s break down some key considerations.
First off, what does long-term mean? When you’re thinking about staying on an antidepressant like Lexapro for an extended period—say years—you want to consider not just how it makes you feel now but also any potential effects down the line.
One major point is the side effects. Everyone reacts differently to medications, so while some might experience minimal issues, others can be hit with fatigue, weight gain, or even sexual dysfunction. It’s like playing a game of roulette; you never quite know the outcome until you spin the wheel yourself. And sometimes these effects can actually persist even after stopping medication.
Now let’s talk about withdrawal symptoms. If you’ve been on Lexapro for a while and decide to stop taking it—whether it’s because you’ve felt better or want to try life without meds—you might face some challenges. People often report feeling dizzy, anxious, or having flu-like symptoms when they suddenly stop taking SSRIs. It’s crucial to work closely with your doc if you ever decide to wean off.
Then there’s the consideration of tolerance. Over time, your brain might get used to the medication. What initially worked wonders may not feel as effective after a few years. That means some people might need a dosage adjustment later on or even a switch to another medication altogether.
It’s also vital to think about mental health as a whole. Some people worry that staying on meds forever means they can’t manage their mental health in other ways—like through therapy or lifestyle changes. But honestly? Combining SSRIs with therapy often yields better results than choosing one over the other.
Another crucial aspect is monitoring by your healthcare provider. Regular check-ins with your doctor help ensure that any side effects are managed and that the medication still suits your needs effectively.
Lastly, let’s remember that there are no hard and fast rules here—everybody’s journey is unique. Long-term use may be totally safe and beneficial for one person while being less so for another based on personal health history and response to treatment.
In short, staying on Lexapro long-term can be safe for many people but requires careful consideration of potential side effects, withdrawal symptoms, tolerance issues, and continuous communication with your healthcare provider. What’s most important is finding what works best for you personally while maintaining a solid support system around you. Stay informed and proactive; it makes all the difference!
Understanding Why Anxiety Can Intensify When Starting SSRIs: Key Insights and Tips
Anxiety can be a real pain, right? So, when you’re starting on a Selective Serotonin Reuptake Inhibitor (SSRI) for that anxiety, it can feel like things are getting worse before they get better. Let’s break this down and see why that happens.
First off, SSRIs work by increasing serotonin levels in your brain. Serotonin is like the brain’s happy juice. It helps regulate mood, anxiety, and even sleep. But here’s the twist: when you first start taking SSRIs, your brain needs to adjust to this new influx of serotonin. This adjustment period can sometimes make anxiety feel more intense.
So what happens? Well, your brain’s receptors are trying to figure out how to react to all this new serotonin. It’s like suddenly throwing a huge party and expecting everyone to know how to dance right away. They need time! That might explain why some people experience heightened anxiety or even new side effects when they start SSRIs.
Another thing worth mentioning is that SSRI effects take time. Typically, it could take several weeks—like 4-6 weeks—for the medication to really kick in. During this waiting game, you might find your anxiety peaking at times because your body is adjusting but hasn’t fully settled down yet.
Plus, there’s often a psychological factor at play too. If you’re excited about getting help but anxious about the side effects or whether it will work at all, you’re putting more pressure on yourself. And that pressure can lead to increased feelings of anxiety.
You might also experience what’s called “activation syndrome.” This means feeling more agitated or restless as the medication starts working its magic on those neurotransmitters. It sounds wild, but it’s pretty common!
Here are some key insights:
- Expect an adjustment period. Give yourself grace; it’s normal for things to get messy initially.
- Communicate with your doctor. They can help navigate through these early bumps in treatment.
- Consider adding therapy. Pairing SSRIs with talk therapy often helps ease the transition.
- Practice self-care. Focus on relaxation techniques like deep breathing or mindfulness during these early stages.
You know that feeling when you finally make it through a tough workout? You feel accomplished but also sore afterward. Starting SSRIs can feel like that—uncomfortable at first but worth it in the long run if you’re committed.
So if you’re starting on an SSRI and noticing your anxiety spiking up instead of calming down, remind yourself it’s just part of the process for many folks—and seriously don’t hesitate to reach out for support during this journey!
So, let’s talk about SSRIs and anxiety. You know, selective serotonin reuptake inhibitors. They’re one of those go-to medications when people are dealing with depression or anxiety. But here’s the thing: even though they help a ton of folks feel better, there’s a bit of a twist that can leave you scratching your head.
Picture this: Sarah, who’s been struggling with anxiety for years, finally decides to give SSRIs a shot after trying everything under the sun—therapy, meditation, yoga (you name it). At first, it feels like she’s found the golden ticket! Her panic attacks start to fade; she feels more relaxed and able to go out without feeling like the walls are closing in. Sounds great, right? But then…bam! She starts experiencing side effects like nausea and insomnia. Her anxiety isn’t just about those panic attacks anymore; now she feels anxious about these new symptoms!
That paradox is really something—SSRI treatment can ease anxiety but also create its own set of worries. It’s like a double-edged sword. Some people end up feeling worse before they feel better, which can be so frustrating and confusing. You think you’re taking a step forward only to find yourself two steps back.
What’s going on here? Well, our brains are complicated. SSRIs work by increasing serotonin levels—which is often called the «feel-good» chemical—but how that interacts with anxiety disorders isn’t straightforward at all. Anxiety isn’t just about brain chemistry; it’s woven into our thoughts, experiences, and even our bodies in ways we don’t fully understand yet.
Plus, everyone’s body reacts differently! What works like magic for one may flop for another or even make things trickier. That variability is part of what makes mental health so…well, messy sometimes! It can feel like an endless cycle of experimenting until you hit upon something that actually helps.
So yeah, while SSRIs have helped millions manage their anxiety symptoms successfully over time (for some people they’re game-changers), they aren’t always the perfect solution for everyone—definitely not an “easy fix.” And that’s why it’s vital to stay connected with your healthcare provider during this journey. Sharing what you’re going through can lead you toward alternatives or additional support if needed.
It all boils down to this: managing anxiety takes patience and understanding—from both yourself and the systems around you. So if you’re navigating through this challenge right now? Just remember—you’re not alone in this paradoxical world of meds and emotions.