You know when you’re trying to figure out how to help someone but there’s just too much information out there? Yeah, it can feel overwhelming.
That’s where the Stetler Model comes in. It’s like having a roadmap when you’re lost, guiding you through the twists and turns of mental health practice.
Basically, it helps professionals turn research into real-world action. You see, it’s all about making sure the stuff that works gets used in therapy.
So if you’re curious about how this approach can make a difference, stick around. We’re gonna break it down together!
Exploring the Benefits of the Stetler Model in Mental Health Practice
The Stetler Model is a big player in the mental health field when it comes to evidence-based practice. It’s like a roadmap for professionals to guide their decisions using scientific evidence, clinical expertise, and patient preferences. Using this model can really amp up the quality of care you get.
One of the key benefits is that it encourages a collaborative approach. Mental health isn’t just about what the therapist thinks is best; it’s also about you and your experiences. This model really stresses teamwork, so both you and your provider are on the same page. When you feel heard, it can totally make a difference in your treatment experience.
Structured Decision-Making is another big win with the Stetler Model. This model outlines steps to evaluate research findings and apply them practically. Think about it this way: when your therapist systematically assesses available evidence before deciding on a treatment plan, it’s like having a GPS versus a paper map—much less chance of getting lost!
Consistency in practice is crucial too. With Stetler’s emphasis on systematic reviews, therapists are encouraged to check out current research and adapt their methods accordingly. That means they stay updated with what actually works, which can lead to better outcomes for you as a client.
What often happens in mental health care is that some methods can become outdated or rely too much on personal preference rather than solid evidence. But with this model, there’s an expectation of ongoing education. Therapists are nudged to keep learning and evolving their techniques based on new information.
Adaptability stands out as well. The Stetler Model isn’t rigid; it’s flexible enough to fit different settings and populations. Whether it’s outpatient services or community mental health centers, each environment can tweak how they implement these principles based on their specific needs.
Lastly, you’ve got patient-centered outcomes. When clients are more involved in decision-making processes thanks to this model, they’re more likely to stick with their treatment plans and feel satisfied with care overall. High engagement usually translates into better outcomes—everyone wins!
So yeah, using the Stetler Model isn’t just some fancy framework; it has real benefits for mental health practice that ultimately serve you better as someone seeking help. It makes everything more effective while putting you right at the center of the process!
Understanding the 5 Phases of the Stetler Model: A Guide to Evidence-Based Practice in Mental Health
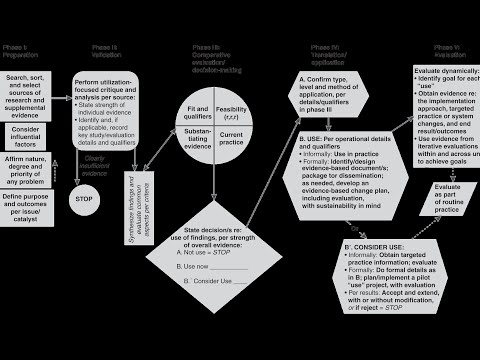
The Stetler Model is one of those frameworks that can really make a difference in mental health practice. Basically, it helps professionals apply research in a way that’s useful. It breaks things down into five phases. Let’s go through each phase, so you get the full picture.
Phase 1: Preparation for Use
In this phase, the focus is on getting ready to implement evidence-based practices. You first need to identify a specific problem or need within your practice. For instance, maybe your clients are struggling with anxiety management techniques. So, you’d start looking for research that addresses effective strategies for that issue. The goal here is to prepare yourself and your team for what’s coming.
Phase 2: Validation
Once you’ve found potential research to use, validating it is key. This means checking if the evidence is credible and relevant to your situation. You want to ask questions like: Is this study from a trusted source? Does it apply to my clientele? If you’re working with teens, but the research focuses on adults, then it might not be valid for your needs at all.
Phase 3: Comparative Evaluation
Here’s where you start comparing the evidence you’ve gathered against what’s currently being done in practice. You’ll weigh the benefits and limitations of both approaches. Maybe you’ve been using traditional talk therapy for anxiety but find cognitive-behavioral techniques backed by strong evidence are more effective. This phase allows you to see which method could be better suited to help your clients.
Phase 4: Decision-Making
Now that you’ve evaluated your options, it’s time to make some solid choices! Ask yourself if you’re ready to switch methods based on the solid evidence you’ve found. Will you implement those cognitive-behavioral techniques instead? Consider how these changes will affect both client outcomes and workflow in your practice.
Phase 5: Application
Finally, we reach implementation! This phase isn’t just about applying new methods; it’s also about monitoring how things go after making changes. It’s crucial to check back periodically—do clients seem happier or more engaged with their treatment? If not, maybe it’s time to revisit previous phases and tweak things until they fit better.
So there you have it—a quick glance at the five phases of Stetler’s Model and how they can guide mental health practices towards evidence-based approaches! It’s all about making informed decisions that improve client care while ensuring everything runs smoothly in practice settings. Pretty neat, right?
Mastering Evidence-Based Practice: 5 Essential Steps for Effective Implementation
When it comes to mental health practice, getting your evidence-based practices down pat can really make a difference. Mastering evidence-based practice, especially through models like Stetler’s, is all about improving patient care by using the best available information. So let’s break down some essential steps for effective implementation.
1. Identify the Need
First things first, you gotta know what you’re working with. You start by looking at current practices and identifying gaps or areas that need improvement. For instance, if your team notices that clients with depression aren’t responding to treatment as hoped, that’s a red flag. You’ll want to gather data on their outcomes and figure out why things aren’t clicking.
2. Gather Evidence
Once you’ve figured out what’s not working, it’s time to dig into the research. Look for studies or data that show what works best in similar situations—this is where evidence-based practice really shines! Let’s say you find a study showing that cognitive-behavioral therapy (CBT) has great results for depression; this could guide your approach moving forward.
3. Assess Applicability
Now, just because something worked elsewhere doesn’t mean it will work for you. You’ve got to check whether the evidence actually applies to your specific situation and client population. For example, if you’re working in a community with unique cultural considerations, you might need to adapt CBT strategies so they resonate better with your clients.
4. Implement Changes
This is where the rubber meets the road! With all that prep work behind you, it’s time to put everything into action. Start small—maybe trial run your new strategy with a few clients before rolling it out fully across your practice. During this phase, keep communication open among staff so everyone knows what’s happening and can share feedback.
5. Evaluate Outcomes
Finally, after implementation comes evaluation—you can’t forget this part! This step is about checking if the changes made any difference in client outcomes and overall satisfaction with care. If you see improvements? Awesome! But if not? Don’t be discouraged; use what you’ve learned to tweak and adjust your approach.
Just like when my friend Sam switched his therapy techniques after realizing his clients weren’t feeling helped by traditional methods—he was nervous at first but eventually found a mix of approaches that sparked real change!
Adopting the Stetler model can feel like a lot sometimes, but following these steps can give structure to making evidence-based changes in mental health settings. Seriously, it’s all about staying flexible and responsive—you know? It’s not just about data; it’s also about people and how we connect with them through our treatment strategies.
So, let’s chat about the Stetler Model for a sec. It’s one of those frameworks that aims to bridge the gap between theory and practice in mental health care. When you’re working in this field, you know how vital it is to actually apply what you learn from research into real-world scenarios, right?
You see, the Stetler Model lays out a process for making that connection more seamless. Basically, it guides practitioners through different phases—from assessing what evidence is available to deciding how best to implement it in their daily routines. It’s like having a roadmap when you’re trying to navigate through the complex highway of mental health treatments.
I remember this one time in therapy school when we were discussing real-life applications of theories. One of my classmates shared her struggle with implementing new techniques she’d learned about anxiety treatment with clients who were hesitant about changes. It struck me how tough that transition can be!
The Stetler Model encourages professionals to not just dive headfirst into new stuff without considering what’s truly relevant for their clients. It makes sense, right? You want to make sure what you’re offering matches up with what your clients need and are comfortable with. For example, if you’re introducing a new cognitive-behavioral technique but your client is still stuck on traditional talk therapy, maybe it’s time to slow down and find a way that blends both worlds.
I guess what I’m saying is, using a model like Stetler’s feels kind of empowering—it’s like giving therapists tools not just for cutting-edge treatment but also for listening and adapting based on individual needs. And let’s face it: every client comes with their own unique story and set of challenges.
Overall, putting the Stetler Model into practice can be a game-changer—it nudges us towards being not just service providers but also partners in our clients’ journeys toward better mental health. And honestly? That’s what it’s all about: creating an environment where people feel seen and heard while also benefiting from the latest in psychological research.